Diabetic Foot Ulcers
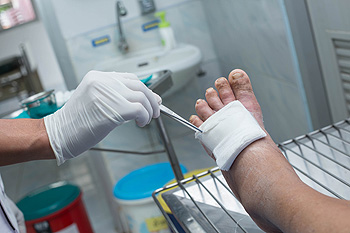
If one’s diabetes is not carefully managed through diet, exercise, and insulin treatment, an all-too-common complication can be a foot ulcer. Ulcers develop because skin tissue breaks down and layers of skin underneath are exposed due to poor circulation, high blood sugar, nerve damage, and irritated or hurt feet. Foot ulcers usually develop under big toes or the balls of the feet. Symptoms to watch for are unusual swelling, irritation, redness, discoloration, drainage from the foot, and odors emanating from the feet. The most visible sign of a foot ulcer is when black tissue (known as “eschar”) surrounds the ulcer because of poor blood flow to the area. However, signs of a foot ulcer are not always present or obvious. Good foot care, including wearing properly fitting, quality shoes, maintaining good foot hygiene, proper trimming of toenails, as well as attention paid to other aspects of physical health, such as heart and kidney disease and obesity, can help with the prevention of foot ulcers. Treatment depends on the cause and severity of the ulcer. It is highly suggested to consult with a podiatrist for proper diagnosis and to obtain a treatment plan.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with one of our podiatrists from Pennsylvania. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Unsightly Cracked Heels
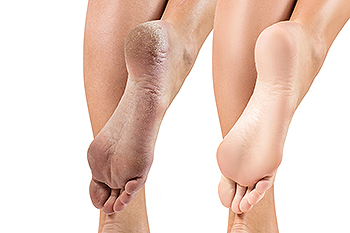
Medical conditions that can include psoriasis and eczema may lead to unsightly cracked heels. It is an ailment that is caused by dry skin, and it can happen for a variety of reasons. The skin on the heels can become dry and cracked from wearing shoes that do not have a back, standing on hard surfaces for the majority of the day, or from living in a dry climate. It may be beneficial to drink plenty of fresh water daily, in addition to applying a good moisturizer on the feet before bed. In severe cases, cracks can cause pain and discomfort. Many patients find it helpful to wear shoes that are closed to protect the skin on the heels. If you suffer from this condition, it is suggested that you schedule an appointment with a podiatrist who can effectively treat this condition.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact one of our podiatrists from Pennsylvania. Our doctors can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Solutions for Cracked Heels
Cracked heels may make you want to think twice about showing off your feet in warmer weather. However, cracked heels may be harmful to more than just the appearance of your feet. If deep fissures and cracks develop in your heels, they may make walking and standing painful for you. Additionally, these openings make way for germs to enter through your skin and cause infection.
There are several different causes of cracked heels. One of the most common reasons for this ailment is dry skin. This problem may make your keeps feel rough tight and itchy. Dry skin may be caused by cold air, extremely hot water, harsh soaps, and aging. Skin disorders such as eczema and psoriasis may eventually lead to dry skin. In some cases, complications may arise from cracked heels. Some of these complications are a loss of feeling in the heel, cellulitis, or a diabetic foot ulcer.
There are ways you can try to prevent getting cracked heels. One of the best ways to do so is to avoid wearing flip flops and sandals because these shoes increase your risk of drying out your feet. You should also avoid wearing shoes with a tall skinny heel, because these shoes cause your heel to expand sideways. At night, you should slather on a thick moisturizing cream on your feet and then cover them in socks to keep your feet moisturized overnight. Drinking water to stay hydrated is also a good way to ensure that your skin doesn’t become dry.
If you suffer from a severe case of cracked feet, you should make an appointment with your podiatrist to see what treatment methods are best for you.
Two Types of Shockwave Therapy
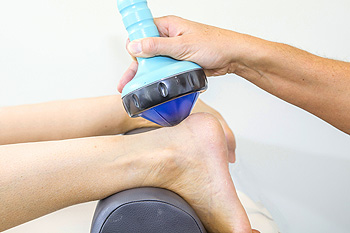 Patients who experience chronic foot pain may benefit from a treatment known as shockwave therapy. Research has shown it may be a helpful remedy for people who have plantar fasciitis. There are two types of this form of therapy, referred to as high and low-energy shock wave treatments. The latter is not painful to administer and may be given in a series of sessions. High-energy treatments are given in one visit and may cause pain. It can be helpful to have a regional block or general anesthesia given before this is used. The purpose of using shockwave treatments is to cause a healing response. This may help deliver nutrients to the affected area, in addition to causing blood vessel formation. Please consult with a podiatrist if you are interested in learning about shockwave therapy, and if it is an appropriate treatment option for you.
Patients who experience chronic foot pain may benefit from a treatment known as shockwave therapy. Research has shown it may be a helpful remedy for people who have plantar fasciitis. There are two types of this form of therapy, referred to as high and low-energy shock wave treatments. The latter is not painful to administer and may be given in a series of sessions. High-energy treatments are given in one visit and may cause pain. It can be helpful to have a regional block or general anesthesia given before this is used. The purpose of using shockwave treatments is to cause a healing response. This may help deliver nutrients to the affected area, in addition to causing blood vessel formation. Please consult with a podiatrist if you are interested in learning about shockwave therapy, and if it is an appropriate treatment option for you.
Shockwave therapy is a treatment commonly used to treat various injuries and conditions, particularly plantar fasciitis in the feet. To learn more, consult with one of our podiatrists from Pennsylvania. Our doctors can provide the care you need to keep you pain-free and on your feet.
Shockwave Therapy
Shockwave therapy is a new treatment option designed to treat bone conditions such as tennis elbow, shoulder pain, and others. Shockwave therapy uses high intensity sound waves that are directed to the affected tissues of the body with pinpoint accuracy. The effects are very beneficial, leading to a production of collagen fibers, eliminating inflammation.
Who Benefits from Shockwave?
Shockwave is recommended for patients suffering from heel pain and associated problems. Heel pain is a common condition which can be caused by obesity, overexertion, and spending a substantial amount of time on hard floors with your feet exposed and unsupported.
Fast and Easy
The therapy is actually a simple process that can leave patients feeling better the very next day. Shockwave therapy is not as dramatic as it sounds. It enables more blood flow to effected areas, addressing the source of the problem and allowing treatment to last for a long time.
Treatment & Recovery Time
Shockwave treatment will enable your feet to recover quickly. This is especially important since surgery is not required. It is cost effective and does not require the use of anesthesia. This treatment is a better option to surgery, since it is proven safe.
If you have any questions, please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Treating Heel Pain with Shockwave Therapy
Shockwave therapy is one treatment option for plantar fasciitis, a condition that causes heel and foot inflammation and pain. This type of injury is often caused by overworking the feet. Heel pain is most common in people that exercise often, individuals who are overweight, and people whose profession require them to stand for long periods of time.
Heel pain can be caused by a number of problems including ill-fitting shoes, strenuous exercise routines or work hazards. Simple treatment options involve buying new shoes, taking ibuprofen, doing heel and foot exercises, and resting your feet. For severe cases, shockwave therapy can be considered a more viable form of treatment.
Shockwave therapy should be considered for patients that have had unsuccessful treatment or whose heel pain has lasted for more than six months. In shockwave therapy, a device delivers shockwaves to the patient’s body, which jumpstart the body’s repair mechanisms. These mechanisms then begin working more effectively to repair damage done to the heel area.
Shockwave therapy also helps eliminate pain in the heel area. When the body’s natural repair mechanisms are triggered, tissue healing in the body is sped up. This leads to pain reduction after pain transmission nerves are stimulated.
Shockwave therapy eliminates the risk factors associated with surgery, such as the use of anesthetics, and is less invasive. Since this technique also helps improve the body’s natural healing techniques, recovery time should be shorter than surgical procedures.
Discomfort issues can also be a side effect of treatment. Short-term issues normally include skin bruising, minor pain during and after treatment, swelling of the heel, and discolored tissue. However, these side effects of shockwave therapy usually disappear after a few days. The fast recovery time of shockwave therapy makes it easy for patients to return to their daily routines.
Like most types of treatments, surgeries, and medications, shockwave therapy is not for everyone. Potential patients with heart conditions and people with pacemakers should not be considered for this technique. People on certain types of medications, usually medications affecting blood clotting, would be ineligible for shockwave therapy. Children and pregnant women should avoid this treatment option as well.
Overall, shockwave therapy could be a great option for heel pain. It is less invasive than surgery, helps trigger natural healing mechanisms, and should be considered by people who have had long bouts of heel pain or tried conventional treatment options that were unsuccessful.
Athlete’s Foot Can Be Uncomfortable
 A common location for patients to notice athlete's foot is between the toes. The symptoms can be uncomfortable and typically include severe itching, tingling, and possibly small blisters. Other places where athlete’s foot can appear are the bottom or sides of the foot. It is known to be contagious, and the fungus that causes this condition lives and thrives in warm and moist environments. These can include locker rooms, public swimming pools, and shower room floors. It can be spread by sharing towels, socks, and shoes. Additionally, many people wear appropriate shoes while in these types of areas as a preventative measure. If you have athlete’s foot, it is strongly suggested that you are under the care of a podiatrist who can successfully treat this condition.
A common location for patients to notice athlete's foot is between the toes. The symptoms can be uncomfortable and typically include severe itching, tingling, and possibly small blisters. Other places where athlete’s foot can appear are the bottom or sides of the foot. It is known to be contagious, and the fungus that causes this condition lives and thrives in warm and moist environments. These can include locker rooms, public swimming pools, and shower room floors. It can be spread by sharing towels, socks, and shoes. Additionally, many people wear appropriate shoes while in these types of areas as a preventative measure. If you have athlete’s foot, it is strongly suggested that you are under the care of a podiatrist who can successfully treat this condition.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact one of our podiatrists from Pennsylvania. Our doctors will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete's Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
What Is Gout Caused By?
Crystals that form between the joints in the big toe can lead to a condition that is known as gout. It can travel to other parts of the body, and it generally begins with the big toe. It is caused by excess uric acid in the bloodstream and lodges between the joints. It often causes debilitating pain, discomfort, and difficulty walking. Uric acid build-ups can be caused by eating foods that have high levels of purines. These types of foods include shellfish, red meat, excess alcohol, and drinks that have a high sugar content. Additionally, gout attacks may be caused by genetic factors, and it is helpful to take measures that can control these episodes. Gout can possibly be controlled by maintaining a healthy weight, and incorporating an exercise routine into the daily regime. It is important that you are under the care of a podiatrist who can properly diagnose gout, and offer the best treatment solutions for you.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact one of our podiatrists from Pennsylvania. Our doctors will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.