Ankle Sprains
Ankle sprains occur when ligaments that support the ankle stretch beyond their limits and tear. These types of injuries are very common and can occur in people of all ages. Sprains may range from mild to severe, depending on how much damage is done to the ligaments. If a sprain goes untreated, a more severe sprain may occur which can further damage the ankle. Repeated ankle sprains can lead to chronic ankle pain.
There are some risk factors that can increase your risk of suffering a sprained ankle. Those who participate in sports, walk on uneven surfaces, have a prior ankle injury, are in poor physical condition, or wear improper shoes are more likely to get a sprained ankle.
There are a few symptoms to look out for if you suspect you are suffering from a sprained ankle. Some common symptoms are swelling, bruising, tenderness, and instability of the ankle. In cases where the tearing of the ligaments is severe, there may be a “popping” sound when the strain occurs.
The RICE method is proven to be effective in treating ankle sprains. RICE stands for Rest, Ice, Compression, and Elevation. Rest is important for treatment, especially within the first 24 to 48 hours. You should also ice your sprained ankle for the first 48 hours for 20 minutes at a time. A small piece of cloth should be placed between the ice and the affected area. For the compression step, you should wear a brace that is snug, but not too tight that it cuts off circulation. When choosing a brace, be sure to choose one that is suitable for the type of ankle sprain you have. Lastly, you should elevate your foot above the heart as often as possible.
After you treat a sprain, you should go through rehabilitation to prevent the injury from occurring again. There are three phases to the rehab process. The first phase involves resting, protecting, and reducing the swelling of the injury. The second phase consists of restoring the ankle’s flexibility, range of motion, and strength. The third phase consists of slowly returning to activity and maintenance exercises.
If you suspect you have an ankle sprain, you shouldn’t hesitate to consult with your podiatrist. Your podiatrist will be able to give you a proper diagnosis and a suitable treatment option for your condition.
The Three Types of Athlete's Foot
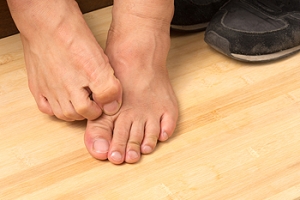
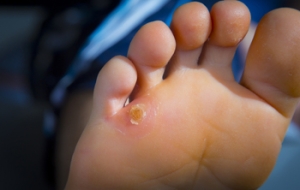
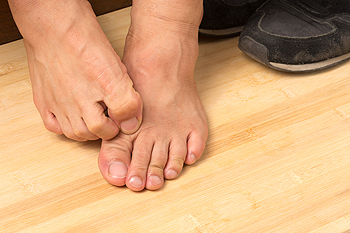 Athlete’s foot is a contagious fungal infection of the skin of the feet. It can cause symptoms such as red, flaky, peeling or cracking skin on the feet, itching, blistering, and a red, scaly rash. There are three types of athlete’s foot. Interdigital athlete’s foot occurs between the toes, often affecting the area between the two smallest toes. Moccasin athlete’s foot starts on the sole of the foot and causes the skin there to thicken and crack before the infection spreads further up the foot. Vesicular athlete’s foot is characterized by the appearance of fluid-filled blisters on the sole of the foot. If you have athlete’s foot, it is suggested that you see a podiatrist for treatment.
Athlete’s foot is a contagious fungal infection of the skin of the feet. It can cause symptoms such as red, flaky, peeling or cracking skin on the feet, itching, blistering, and a red, scaly rash. There are three types of athlete’s foot. Interdigital athlete’s foot occurs between the toes, often affecting the area between the two smallest toes. Moccasin athlete’s foot starts on the sole of the foot and causes the skin there to thicken and crack before the infection spreads further up the foot. Vesicular athlete’s foot is characterized by the appearance of fluid-filled blisters on the sole of the foot. If you have athlete’s foot, it is suggested that you see a podiatrist for treatment.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact one of our podiatrists from Pennsylvania. Our doctors will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How to Deal with Athlete's Foot
Athlete’s foot is a type of fungal infection that affects the skin on the feet. It is caused when the tinea fungus grows on the foot. It is possible to catch the fungus through direct contact with someone who has it or by touching a surface that is contaminated with it. This type of fungus thrives in warm, moist environments such as showers, locker room floors, and swimming pools. Your risk of getting it may also increase by wearing tight-fitting, closed-toe shoes, or by having sweaty feet.
Symptoms of athlete’s foot include itching, stinging or burning sensations between the toes. You may also experience toenails that are discolored, thick, crumbly, or toenails that pull away from the nail bed.
Your podiatrist may diagnose athlete’s foot by detecting these symptoms or by doing a skin test to see if there is a fungal infection present. The most common exam used to detect Athlete’s foot is a skin lesion potassium hydroxide exam. To use this method, your doctor will scrape off a small area of the infected skin and place it into potassium hydroxide. The potassium hydroxide will destroy the normal cells and leave the fungal cells untouched so that they are visible under a microscope.
There are a variety of treatment options for athlete’s foot. Some medications are miconazole (Desenex), terbinafine (Lamisil AT), clotrimazole (Lotrimin AF), butenafine (Lotrimin Ultra), and tolnaftate (Tinactin). While these options may be able to treat your fungus, it is best that you consult with a podiatrist in order to see which treatment option may work best for you.
In some cases, Athlete’s foot may lead to complications. A severe complication would be a secondary bacterial infection which may cause your foot to become swollen, painful, and hot.
There are ways that you can prevent athlete’s foot. Washing your feet with soap and water each day and drying them thoroughly is an effective way to prevent infections. You also shouldn’t share socks, shoes, or towels with other people. It is crucial that you wear shower sandals in public showers, around swimming pools, and in other public places. Additionally, you should make sure you wear shoes that can breathe and change your socks when your feet become sweaty. If you suspect that you have Athlete’s foot, you should seek help from a podiatrist as soon as possible.
What Causes Achilles Tendon Injuries?
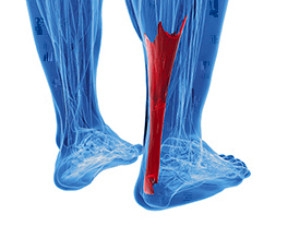
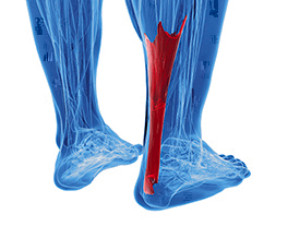 The Achilles tendon is the thick band on the back of the ankle that connects the calf muscle to the heel bone. Achilles tendon injuries are often overuse injuries or sudden traumas. One common injury, Achilles tendonitis, occurs when the tendon becomes inflamed near its connection to the heel bone. Achilles tendon ruptures are also common, and they can be very painful and may take a long time to heal. Because a lack of flexibility is the most common cause of injury to the Achilles tendon, proper stretching of the lower legs before working out is the most important step to prevent an injury. When healing from the injury, non-impact exercises, such as swimming and cycling, are highly suggested to keep you as in shape as possible. If you have questions about preventing an injury, or you believe you may have injured your Achilles tendon, please consult with a podiatrist.
The Achilles tendon is the thick band on the back of the ankle that connects the calf muscle to the heel bone. Achilles tendon injuries are often overuse injuries or sudden traumas. One common injury, Achilles tendonitis, occurs when the tendon becomes inflamed near its connection to the heel bone. Achilles tendon ruptures are also common, and they can be very painful and may take a long time to heal. Because a lack of flexibility is the most common cause of injury to the Achilles tendon, proper stretching of the lower legs before working out is the most important step to prevent an injury. When healing from the injury, non-impact exercises, such as swimming and cycling, are highly suggested to keep you as in shape as possible. If you have questions about preventing an injury, or you believe you may have injured your Achilles tendon, please consult with a podiatrist.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of Pennsylvania. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Achilles Tendon Injuries
The Achilles tendon is the largest tendon in the body; it is a tough band of fibrous tissue that stretches from the bones of the heel to the calf muscles. This tendon is what allows us to stand on our toes while running, walking, or jumping, it is common for this tendon to become injured. In severe cases, the Achilles tendon may become partially torn or completely ruptured. However, this tendon is susceptible to injury because of its limited blood supply and the high level of tension it endures.
The people who are more likely to suffer from Achilles tendon injuries are athletes who partake in activities that require them to speed up, slow down, or pivot. Consequently, athletes who engage in running, gymnastics, dance, football, baseball, basketball, or tennis are more likely to suffer from Achilles tendon injuries. Additionally, there are other factors that may make you more prone to this injury. People who wear high heels, have flat feet, tight leg muscles or tendons, or take medicines called glucocorticoids are more likely to have Achilles tendon injuries.
A common symptom of an Achilles tendon injury is pain above the heel that is felt when you stand on your toes. However, if the tendon is ruptured, the pain will be severe, and the area may become swollen and stiff. Other symptoms may be reduced strength in the lower ankle or leg area, and reduced range of motion in the ankle. When the Achilles tendon tears, there is usually a popping sound that occurs along with it. People who have acute tears or ruptures may find walking and standing to be difficult.
If you suspect you have injured your Achilles tendon, you should see your podiatrist to have a physical examination. Your podiatrist will likely conduct a series of tests to diagnose your injury including a “calf-squeeze” test. Calf squeeze tests are performed by first squeezing the calf muscle on the healthy leg. This will pull on the tendon and consequently cause the foot to move. Afterward, the same test will be performed on the injured leg. If the tendon is torn, the foot won’t move because the calf muscle won’t be connected to the foot.
When Should I See a Foot and Ankle Surgeon?
 Most injuries and diseases of the foot and ankle are not treated surgically. However, a foot and ankle surgeon can still help you by examining your feet and ankles when you experience pain or other symptoms of injury or disease. You may want to consult a foot and ankle surgeon if you have sustained an injury, such as a sprain or fracture, have a medical condition that can affect the feet, have difficulty completing daily activities, or notice a change in the appearance of your feet or ankles. Foot and ankle surgeons tend to only suggest surgery when a problem is severe and non-surgical treatments have failed. For more information about how a foot and ankle surgeon may be able to help you, please consult with a podiatrist.
Most injuries and diseases of the foot and ankle are not treated surgically. However, a foot and ankle surgeon can still help you by examining your feet and ankles when you experience pain or other symptoms of injury or disease. You may want to consult a foot and ankle surgeon if you have sustained an injury, such as a sprain or fracture, have a medical condition that can affect the feet, have difficulty completing daily activities, or notice a change in the appearance of your feet or ankles. Foot and ankle surgeons tend to only suggest surgery when a problem is severe and non-surgical treatments have failed. For more information about how a foot and ankle surgeon may be able to help you, please consult with a podiatrist.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact one of our podiatrists of Pennsylvania. Our doctors will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Foot and Ankle Surgery
When conservative, noninvasive methods prove ineffective, surgery may be selected as the next course of action for the treatment of your foot or ankle condition. A wide number of foot and ankle surgical procedures exist, and it is up to your podiatrist to determine which intervention will be most appropriate and helpful for your case. Some surgical procedures include bunion surgery, fusion, hammertoe surgery, heel spur surgery, metatarsal surgery, nail surgery, neuroma surgery, reconstructive surgery, skin surgery, and tendon surgery. Typically, surgery is turned to as a definitive way to alleviate excessive pain or discomfort and to return your foot to full mobility.
Regardless of the location on the body, all surgical procedures require preoperative testing and examination to ensure the surgery’s success and preferred outcome. A review of your medical history and medical conditions will take place, as will an evaluation of any current diseases, illnesses, allergies, and medications. Tests such as blood studies, urinalyses, EKG, X-rays, and blood flow studies may be ordered. Because the procedure involves the foot and/or ankle, the structures of your feet while walking may also be observed by your podiatrist.
Care post-surgery will depend on the type of surgical procedure performed. Typically, all postoperative care involves rest, ice, compression, and elevation. To improve and ensure a safe recovery, your foot and ankle surgeon may also employ the use of bandages, splints, surgical shoes, casts, crutches, or canes. He will also determine if and when you can bear weight. A timely and thorough recovery is a priority for both you and your podiatrist, and carefully following postoperative instructions can help achieve this.
Why Corns May Develop on the Feet
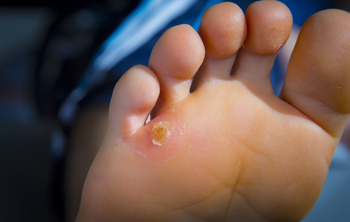 People worldwide can be affected by corns on the feet. They are defined as small, hardened portions of skin that have developed as a result of excess friction. Corns can form on the soles of the feet, or between the toes, and can cause severe pain and discomfort. Additional causes of corns can include wearing shoes and socks that do not fit correctly, and medical conditions consisting of bunions and hammertoes. Mild relief may be found when larger shoes are worn if the corn is between the toes. This may help to prevent further irritation that may happen from the toes rubbing together. The corn may soften after the affected foot is soaked in warm water, and it can help to use a pumice stone to eliminate dead skin on top of the corn. If you have corns on your feet, please consult with a podiatrist who can help you to remedy this condition.
People worldwide can be affected by corns on the feet. They are defined as small, hardened portions of skin that have developed as a result of excess friction. Corns can form on the soles of the feet, or between the toes, and can cause severe pain and discomfort. Additional causes of corns can include wearing shoes and socks that do not fit correctly, and medical conditions consisting of bunions and hammertoes. Mild relief may be found when larger shoes are worn if the corn is between the toes. This may help to prevent further irritation that may happen from the toes rubbing together. The corn may soften after the affected foot is soaked in warm water, and it can help to use a pumice stone to eliminate dead skin on top of the corn. If you have corns on your feet, please consult with a podiatrist who can help you to remedy this condition.
If you have any concerns regarding your feet and ankles, contact one of our podiatrists of Pennsylvania. Our doctors will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctors to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Corns and Calluses
A corn is a lesion that forms in the skin of the foot, and it is typically circular in shape, small in size, and thick and rough in texture. A corn generally occurs as a result of repeated pressure on the skin; one example of this is the rubbing of a shoe against the skin. Corns differ from calluses in that their central cores are harder in texture.
A corn is a relatively common condition with a wide variety of treatment options. If a corn becomes overly uncomfortable or painful, consult with your podiatrist; he can determine the best method of treatment that is appropriate for you. Corns may return if the underlying cause of its development is not treated or removed. Avoid removing corns at home, as improper removal may cause infection.
A callus, similar to a corn, is an area of skin that has become thickened due to repeated pressure and rubbing. The rubbing causes the skin to create a layer of protective skin, which is the formed callus. Calluses can differ in size between people, and they can also become painful.
Multiple treatments are available for calluses. At-home treatment and removal should be avoided, as this can potentially lead to infection. Your podiatrist can best determine the cause of your calluses and suggest the treatment most appropriate for you.